Author: Dr Zamiel Hussain, GP and Founder at AccessGP
Clinical review: Dr Anna Trigell, GPwER in Dermatology
Rosacea is often mistaken for sensitive skin, adult acne, or simply a tendency to flush easily. In reality, it is a common inflammatory skin condition that can cause persistent facial redness, visible blood vessels, and acne-like breakouts, often with a pattern of flare and remission. Because it can overlap with other skin concerns, many people spend months trying products that are not designed for the underlying problem.
This article explores what rosacea is, why it happens, how to recognise it, and when it is sensible to seek medical advice.
About this series: Scratching the Surface of Dermatology
Scratching the Surface of Dermatology is an educational blog series exploring common skin concerns seen in general practice. Articles are written by Dr Zamiel Hussain, Lead GP and Founder of AccessGP. Articles are clinically reviewed by Dr Anna Trigell, GPwER in Dermatology, who leads the AccessGP Skin Clinic.
The series aims to explain skin conditions in a clear, evidence-based way, helping patients understand symptoms, treatment options, and when to seek medical advice.
What is rosacea?
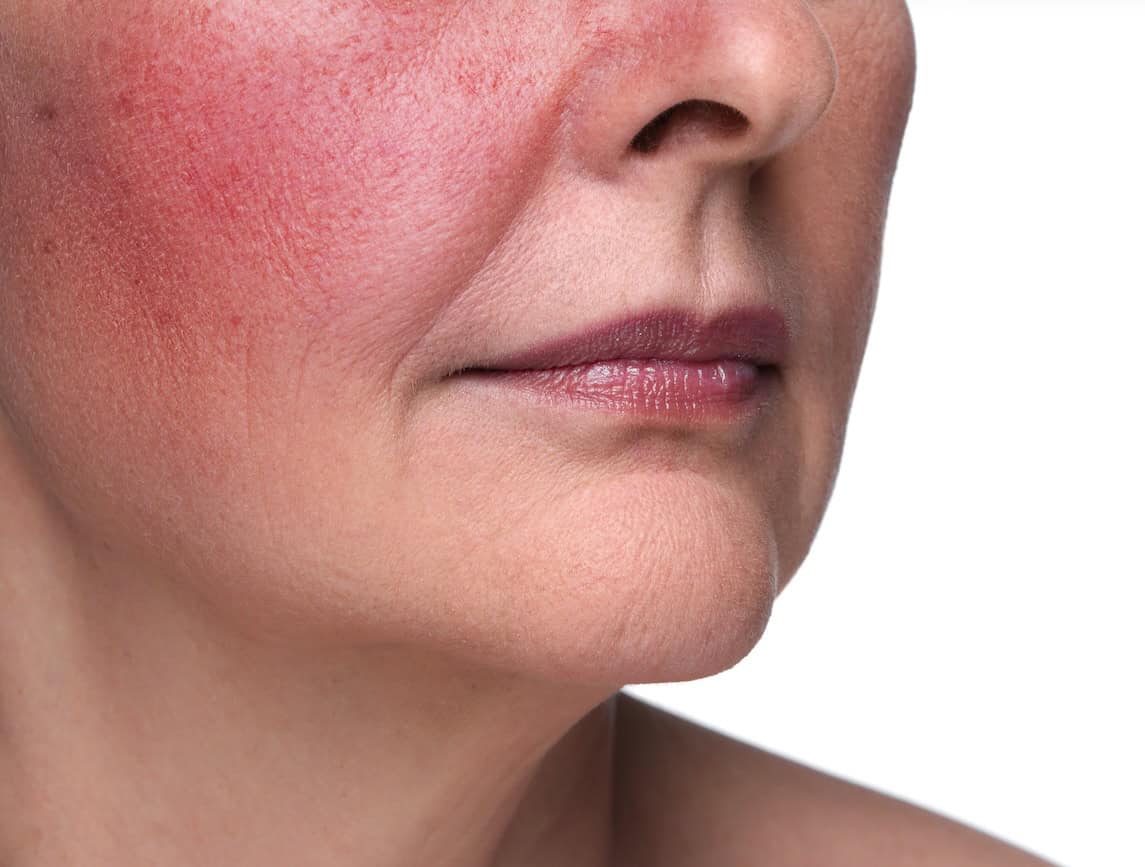
Rosacea is a chronic inflammatory skin condition that primarily affects the central face, particularly the cheeks, nose, chin, and forehead. It usually develops in adulthood and can vary considerably in severity. For some people, it presents mainly as background redness and flushing. For others, it causes more persistent inflammation with red bumps and pustules that can easily be mistaken for acne.
Unlike acne, rosacea is not driven by blocked pores. Instead, it appears to involve a combination of vascular sensitivity, inflammation, and skin barrier dysfunction. This helps explain why redness and flushing are such prominent features.
In some patients, microscopic organisms known as Demodex mites, which naturally live on the skin, are thought to contribute to inflammation through a hypersensitivity reaction. This has led to the development of newer topical treatments that specifically target these pathways and can be effective in managing certain types of rosacea.
Recognising the signs
Rosacea often begins gradually. People may notice that they flush more easily than before, or that their skin remains red for longer after heat, alcohol, exercise, or stress. Over time, the redness can become more persistent.
In many cases, rosacea also causes inflammatory papules and pustules, particularly across the cheeks and nose. This is one reason it is so often confused with acne. The difference is that rosacea tends to sit on a background of redness and sensitivity, and blackheads are not usually a feature.
Some patients also describe stinging, burning, or unusually reactive skin. Standard acne treatments can sometimes make this worse rather than better, especially if they are drying or overly harsh.
Rosacea can also affect the eyes. Ocular rosacea may cause irritation, dryness, watering, or a gritty sensation. If eye symptoms are present, this should be assessed promptly.
Why rosacea is often misdiagnosed
A common pattern in practice is a patient who assumes they have acne and tries to treat it accordingly. They may use exfoliating acids, foaming cleansers, or strong anti-blemish products, only to find that their skin becomes redder, drier, and more inflamed.
That is because rosacea requires a different approach. Acne management often focuses on reducing oil production and preventing blocked pores. Rosacea management is more about calming inflammation, protecting the skin barrier, and reducing vascular and inflammatory triggers.
Getting the diagnosis right matters. It can prevent months of frustration and avoid unnecessary irritation from unsuitable products.
How rosacea is managed
Although rosacea is a chronic condition, it can often be managed very effectively with the right treatment and skin care approach.
A large part of treatment involves identifying and reducing triggers. Common triggers include alcohol, spicy food, hot drinks, temperature extremes, stress, and certain skin care products. Gentle, fragrance-free cleansing and regular moisturising are often important first steps, particularly when the skin barrier has become compromised.
Prescription treatment may include topical therapies that reduce inflammation and, in some cases, target pathways linked to Demodex-related inflammation. For more persistent or widespread inflammatory rosacea, oral treatment may sometimes be appropriate. Where visible thread veins or background redness are prominent, some patients also explore laser-based options, although this is not always necessary.
As with many inflammatory skin conditions, improvement is rarely immediate. Consistency, realistic expectations, and an accurate diagnosis tend to make the greatest difference over time.
When to seek GP advice
It is sensible to seek medical advice if facial redness is becoming persistent, if flushing is frequent or distressing, or if there are acne-like spots that are not improving with standard skin care. Review is also worthwhile if the skin feels increasingly sensitive, stings easily, or seems to worsen with usual acne treatments.
Early assessment can help clarify the diagnosis, guide treatment, and reduce the risk of prolonged irritation from using the wrong products.
How AccessGP Can Help
The AccessGP Online Skin Clinic is led by Dr Anna Trigell, GPwER in Dermatology, and supports patients with a wide range of common skin concerns.
We assess suitability for online dermatology by initial skin concern triage, allowing patients to submit photos and brief details so concerns can be reviewed and directed appropriately. Where suitable, skin conditions can then be assessed through convenient digital consultations using photo and video appointments, avoiding unnecessary delays.
Our clinic focuses on clear diagnosis, evidence-based treatment, and practical skin care plans. Patients are advised when remote management is appropriate and when in-person assessment or specialist referral is needed, ensuring care is both safe and proportionate.
You can also learn more about skin concerns at our Knowledge Base.
Reliable Resources and Clinical References
British Association of Dermatologists (BAD): www.bad.org.uk
NHS: Rocea: www.nhs.uk/conditions/rosacea
NICE Clinical Knowledge Summaries: cks.nice.org.uk